CHICAGO, IL, December 2nd, 2019. According to the Agency for Healthcare Research and Quality, more than 17,000 lawsuits related to pressure injuries are filed annually in the United States, second only to wrongful death lawsuits.
The Centers for Medicare & Medicaid Services (CMS) have acknowledged that some ulcers are unavoidable, which means they can occur despite receiving the best care possible. However, it’s up to the facility to prove they did everything they were supposed to, and despite that, the patient developed that pressure injury.
“To prove unavoidability, proper documentation of best care needs to be in place, as well as documentation that all proper prevention and treatment measures were implemented,” says Heidi Cross, a certified wound specialist who also has her own independent practice as an expert witness for plaintiff and defense attorneys in New York. “That’s where my clients run into trouble, in many cases things were never documented and even if they were, it can be next to impossible to find.”
That’s where Swift’s WoundProof Program comes in. Healthcare facilities that adopt Swift Skin and Wound technology will have a system to collect and manage the proper documentation of skin and wound evaluations, and always be in compliance with clinical regulations and best practices.
The clinical data and reports contained within Swift have already been used successfully many times to ward off claims and litigation. The Swift WoundProof Program protects healthcare organizations through four key components:
- Eliminating avoidable in-house acquired pressure injuries
- Standardized best practice management of non-avoidable in-house acquired pressure injuries
- Workflows that ensure comprehensive, complete, and admissible documentation of all wounds
- Court-ready fast and easy export of all relevant documentation
“If a facility is using Swift Skin and Wound, they can have the peace of mind that all of that is captured by the software,” says Heidi “Swift really has thought of everything”
The WoundProof program uses Swift Skin and Wound technology to track high-risk patients and alert caregivers immediately to changes in skin integrity to prevent avoidable pressure ulcers from ever occurring. For those pressure injuries that are unavoidable, the solution provides comprehensive evaluations, best practices to clinicians at the point of care and enforceable workflows that together ensure delivery of the best care possible. All of this is documented in a way that it can be easily exported into reports to be used in litigation if it arises. However, most facilities that use Skin and Wound can stop a lawsuit before it even happens because they have this program in place.
“It’s been extremely helpful to work with Heidi on this process, as we’ve been able to identify and build a program that we can be confident in“ says Preethi Vaidyanathan, Product Manager at Swift, “To have someone that deals with these types of cases on a daily basis validating that our solution meets the needs of the healthcare industry, means that we can deliver the exact solution needed to protect organizations from these lawsuits.”
Heidi Cross will be hosting a webinar on the topic “Legal Perils and Pitfalls of Wound Care: How to Keep Your Healthcare Facility Out of Court” on December 12th at 2pm ET. You can register here.
About Swift
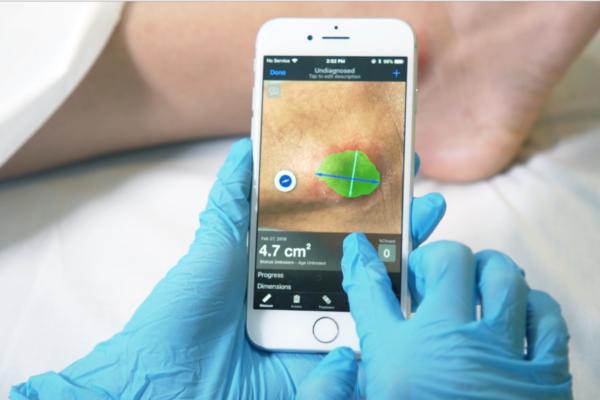
Swift is the world leader in digital wound care management, delivering advanced wound care visualization and touchless measurement through its smartphone-ready Swift Skin and Wound software. Swift streamlines clinical and administrative wound care management workflows, from image capture and automatic risk scoring to assessment scheduling and claims submission. Today, Skin and Wound is in use by more than 2,000 healthcare facilities to monitor over 200,000 patients and streamline over $1 billion in reimbursements. To learn how Swift has digitized and transformed wound care, visit swiftmedical.com.
About Heidi Cross
Heidi H. Cross, MSN, RN, FNP-BC, CWON, is a board-certified Wound and Ostomy Nurse and a board-certified Family Nurse Practitioner in Syracuse, NY. She is a graduate of Syracuse University, with a Master’s Degree in Nursing from the State University of New York Upstate Medical University.
She has extensive experience caring for wound and ostomy patients in both acute care and in long-term care facilities. Currently, she is employed by CNY Surgical Physicians consulting for nursing homes in the Syracuse area and has her own independent practice as an expert witness for plaintiff and defense attorneys.
She participated in developing the National Pressure Ulcer Advisory Panel’s Clinical Practice Guidelines for Prevention and Treatment of Pressure Ulcers in 2014.