A patient recently showed up in the hospital where I work, with a Christmas ornament embedded so deeply in his foot I felt the bone underneath when I extracted it. Unfortunately, this patient couldn’t seek medical help right away. Consequently, his wound got so infected that most of the tissue around it died and we had to amputate his foot.
Most people are horrified when they hear this story, but they can also relate. Everyone has a wound story — a slice from a kitchen knife that slipped their grasp, a scraped knee, or perhaps a paper cut that, as tiny as it was, stung for days.
Now, imagine what these injuries would be like if they healed slowly, or not at all. Imagine living every day with a raw, gaping hole in one or more areas of your body. That’s the sad reality for millions of people around the world — many of whom are elderly or who have serious illnesses — who suffer from chronic, acute or traumatic wounds.
Wounds are a big global problem — one that isn’t as discussed or researched as often as, say, cancer or heart disease. Since wounds are often the symptoms of underlying conditions like diabetes and CVD, there is no clinical specialty dedicated to wound care. However, by conservative estimates, there are at least nine times more people around the world with chronic and serious wounds than there are people living with cancer.
In the United States alone, more than 8.2 million patients who receive Medicare benefits have chronic wounds. This hurts more than patients; it also puts great strain on healthcare resources. Medicare, for one, spends as much as $96.8 billion annually on wound treatment.
The wound problem is expected to get worse as populations age and experience higher rates of chronic diseases such as diabetes, heart disease and obesity — conditions that are linked to a higher risk for chronic wounds. Over the next decade, the incidence of chronic wounds is expected to rise at a rate of 2% annually. So, why can’t doctors just put a bandage on these wounds and send the patients home with a prescription?
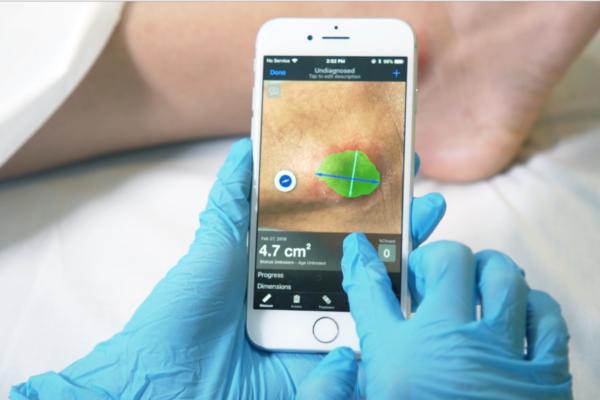
If only it were that simple. Chronic wounds are complex, and the key problems with wound care are both clinical and systemic. Diagnosing and treating chronic wounds requires accurate measurement of wound area and depth, as well as reliable analysis of the tissue surrounding the wound. Yet, most wound assessments today are done with a paper ruler to measure area size and a cotton swab to gauge depth. This method generally produces inaccurate data and can be uncomfortable, even painful, for wound patients.
From a systemic perspective, a major problem is the lack of clarity around who should be responsible for wounds. If a diabetic patient develops a foot ulcer, for instance, does the treatment and care for this wound fall to the endocrinologist or should the patient be referred to a vascular specialist? Should a home health nurse with little or no training in wound care — which sometimes involves delicate tasks such as debridement or removal of damaged tissue — be responsible for ongoing monitoring and management of a chronic wound?
The confusion over responsibility for wound care gets even worse when patients have multiple health problems. Is it the surgeon, cardiologist, endocrinologist or orthopedic specialist who should be looking after the post-surgical wound of a patient with heart disease and diabetes?
Many of these medical specialists have neither the time nor the inclination to look after a chronic wound. It’s simply not in their wheelhouse, and most healthcare funding models don’t provide additional compensation for the care of complex wounds. For patients, all of these challenges can translate to lower quality of care, due in large part to the lack of continuity of care for their wounds.
There are potential solutions. At the Welsh Wound Innovation Centre in Cardiff, Wales, wound patients are looked after by interdisciplinary teams that, depending on the patient’s health history, might include an endocrinologist, vascular surgeon, wound care specialist and home health nurse. To ensure consistency, the center works to ensure patients are seen by the same team each time they visit. While not every jurisdiction can afford to build a similar center, hospitals and clinics would do well to study the Welsh model and see how they can adopt it in their practices.
For such a solution to work, however, healthcare organizations would need to build more wound care expertise among their practitioners. This is why wound care training for all healthcare professionals, regardless of their discipline, should be integrated into medical schools’ curricula and reinforced with further education in clinics and hospitals.
Better methods to assess and manage wounds are also critical, and this is where technology can play an important role. Accurate digital images that show the progression of wound healing also encourages patients to be more engaged in their treatment. In my own research, I’ve found that patients who can see images of their wounds tend to take better care of their wounds. In general, there’s still a lot we as a global medical community don’t know about wounds. We need to encourage — and fund — more research into wound healing. It’s hard to treat what we don’t understand fully.
There isn’t a neat answer to the challenge of chronic wounds. Politicians, healthcare industry leaders, educators, and patients need to push for solutions. Policymakers need to look at how different healthcare delivery and funding models can improve wound care. The hard truth is that the wound problem isn’t going to go away. Even as researchers find advanced treatments for most of today’s serious diseases, people will always be at risk for wounds. That’s why healthcare and technology experts need to start working on solutions today.
To learn how to use digital wound care technology in your wound care program, download our latest whitepaper.
Written by Dr. Sheila Wang is the co-founder and Chief Medical Officer at Swift Medical