Smartphones powered by artificial intelligence (AI) have become an essential part of modern life. They help us navigate traffic, locate services and make recommendations – from restaurants to potential partners. Now these devices have become a potent force in healing diabetic wounds and preventing amputation.
Wounds are a serious health concern. People with diabetes often suffer from reduced sensation, known as diabetic neuropathy, allowing them to wear a hole (wound) in their foot just as they might wear a hole in a sock or shoe. Complicating matters is peripheral artery disease, a condition present in more than half of people with diabetic foot wounds, which makes wounds harder to heal. The result is that even small cuts and abrasions often go unnoticed until they become much more serious.
It is estimated that every 20 seconds someone on the planet loses a limb to diabetes, with foot ulcers serving as ground zero for more than 80% of these amputations.1
Prevailing methods are failing patients
The bottom line is that we need to measure what we manage—and we aren’t doing as good a job as we could. Current methods make this surprisingly difficult to achieve. These involve using a paper ruler to measure length and width and inserting a cotton swab into the wound to measure depth. Not only is this painful, it is often inaccurate given that wounds are typically irregular in shape. Furthermore, this measurement can be wildly inaccurate—with more than 30% interoperator error.2 Tracking the healing process also means monitoring changes in the proportion of healthy tissue relative to unhealthy. This too is equally prone to subjectivity.
Unreliable wound information creates a variety of challenges and can lead to improper diagnosis and treatment. The consequence is patients who simply do not heal, or worse, amputation.
Revolutionizing diabetic wound care
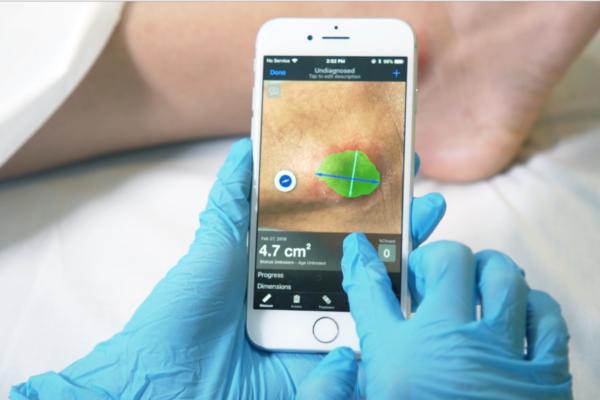
Smartphones powered by machine visioning and AI are changing the game. Now the simple act of taking a picture can make the difference in capturing reliable wound information. Devices with Swift Skin and Wound Digital Wound Care Technology can assess wounds with far more accuracy than even the most seasoned wound care professionals. Over time, this allows caregivers to gauge progress and to ensure the right course of treatment is prescribed.
Diabetes is of course a complex disease. Treatment involves a variety of medical practitioners, from family doctors, and specialists, to nurses and therapists. Capturing wound data digitally brings the added benefit of making it easy to share this information, allowing teams to provide more holistic care. Through automation, treatments can also be standardized using checklists and other prompts. This ensures critical procedures and assessments are delivered consistently.
Putting patients at the center of the healing process
One particularly interesting benefit of AI powered imaging is the impact on patient engagement. A study from the International Wound Journal found that photography is an effective tool in empowering patients in the management of their wounds.3 80% of study participants said photographing their wounds, which can be hard for them to see, would help them track progress without relying solely on the physician’s assessment. More than half reported it would allow them to be more involved in the healing process and better coordinate their own care across health care specialists.
When it comes to overcoming the challenges of diabetic wound care, a picture does indeed speak a thousand words.
If you would like to see how Swift Skin and Wound works you can book a demo .
References
- Chockalingam, Nachiappan. Preventing a Million Diabetic Foot Amputations. The Conversation, 2018.
- Rogers LC, Bevilacqua NJ, Armstrong DG, Andros G. Digital planimetry results in more accurate wound measurements: a comparison to standard ruler measurements. J Diabetes Sci Technol. 2010;4(4):799-802. doi:10.1177/193229681000400405
- Wang SC, Anderson JAE, Jones DVB, Evans R. Patient perception of wound photography. Int Wound J 2014; doi: 10.1111/iwj.12293