After more than 40 years as a leading clinician, researcher and educator in wound care, Professor Keith Harding has plenty to say about this still-evolving field of medicine. He took time recently to share his thoughts on wound healing and to provide perspective on how wound care has evolved over the last four decades.
It was during your final year as a medical student at the University of Birmingham that you became interested in wound care. Can you tell us more about this?
I had asked my mentor at the university, Professor Sir Geoffrey Slaney, if I could do something for him. So he got me working for three months on a project that tried to show if low-dose heparin – which acts as an anticoagulant – affected wound healing. That’s how I got interested in wounds.
How did this lead to your career and expertise in wound care?
After Birmingham I came back to South Wales, where I’m from originally, and got a job as a surgical trainee with Les Hughes, a previous professor of surgery in Cardiff who had invented a modern wound dressing and was running a wound clinic at the University of Wales. After funding for the clinic ran out, I went to work in general practice but continued to run the clinic on a volunteer basis. I was also giving up half my holidays to speak at wound healing meetings. Then at some point I took a six-month sabbatical to look at wound healing in North America. What I found was that in Wales we were seeing a lot patients but not doing research, whereas in North America there was a lot of wound biology research but not as much clinical practice.
As head of the Wound Healing Research Unit at Cardiff University, you’ve driven a number of innovations in wound care. Could you highlight some of these innovations?
We developed the first master’s course in wound healing, and that continues to be offered today by several universities. We also created a quality-of-life tool, called the Cardiff Wound Impact Schedule, that’s now used in at least 50 trials around the world and translated into about 20 languages. This is a questionnaire that patients fill in to report on their quality of life. An algorithm scores and analyzes the responses. It’s a great way to understand what’s really bothering your patient. Instead of just focusing on the biological aspect of wound healing, you can understand how their wound interferes with their quality of life. For example, they may have stopped socializing because their wound is smelly, so you design their treatment to also address the odor to improve their quality of life.
We also have a number of patents, including one for a gene signature innovation that predicts which wounds will heal as well as therapeutic agents that are known to influence the appearance of genes that help in wound healing. The papers on these innovations will be published soon.
What are some of the key lessons you learned as you worked on these innovations?
One of the first thing is, no data equals no problem so we have to go out and capture wound data in terms of numbers and costs. In 2016 we published something to show that in Wales about 330 million pounds a year was spent on wound care – that’s six per cent of National Health Service spend. Without these facts in hand it’s difficult to get government engagement.
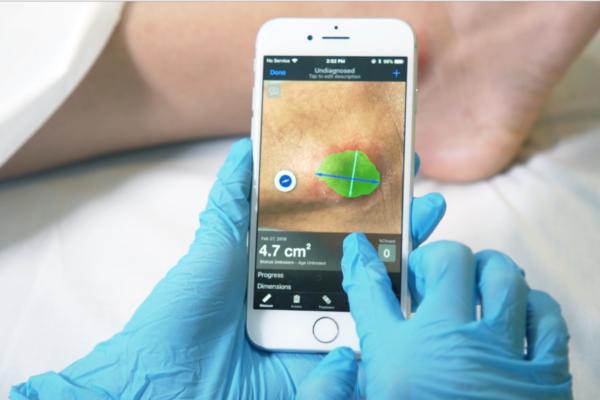
The other thing we’ve learned is the importance of being objective in wound measurement. If you look at patient records, there’s a lot of free-hand entry to indicate that a wound is getting better or worse but there’s little or no measurement or data. This is where Swift comes in.
So how can healthcare facilities be prompted to adopt methods and practices for accurate wound measurement and documentation?
Awareness and education are key. We know that 45 per cent more wound patients are healed when you educate nurses, and 85 per cent more are healed when we assign a buddy such as a nurse educator alongside the nurse.
You recently became the first scientific advisor at Swift. What made you take on this role?
Sheila Wang (chief medical officer at Swift) spent time with me when she was in medical school. When I saw her developing what eventually became Swift Skin and Wound, I knew that this was something that could really make a difference in wound healing.
I’ve seen other solutions in the market that are over-engineered and over-complicated, and there are a couple of devices out there that are probably useful for research studies. But none of them are pragmatic enough for clinicians to collect meaningful data in a routine manner in various patient scenarios. By comparison, Swift Skin and Wound is designed for practical clinical and administrative applications, in ways that are really making a difference for patients and healthcare providers
After 42 years in wound care, you show no signs of stopping. What are some of your current projects?
I’m now at an age where I’m more about evolution than revolution. I’m trying to create a new specialty of “woundology.” Today, if you have a wound who do you see? That could be anybody and everybody. At a time when we have the ability to transplant organs and cure complex diseases, we should also be able to seek help from a professional who knows more than a little bit about wound healing.
We also have government approval in Wales to set up a national wound registry – a project we’ve been working on for a number of years. The ultimate goal behind this registry is to achieve consistency of approach, get data you can interrogate and improve the quality of care that patients get when they have a wound. Because when it comes to wound care, it’s still like the Wild West out there. We’re awash with new treatments but lack understanding of when, where and how to use those treatments to maximize benefits for patients.