Effectively healing and caring for chronic wounds is a complex and often multidisciplinary task. Layered on top of this are the differences in the various sites of service where wound care happens and maintaining proper communication between providers as a patient spans these settings. Hospital in- and outpatient, ambulatory care settings, skilled nursing and home health agencies all play an important role in managing the burden of chronic wounds.
The ambulatory wound care clinic, or wound care specialist, plays an important role in this ecosystem. Often being the referral center from acute and post-acute care settings, the specialists at these clinics see more complex and advanced wounds than any other providers. Given this, the hope for healing and closing chronic wounds often rests under the care of these specialists.
Wound care has historically had small margins for ambulatory wound care providers and, in some settings, is widely regarded as a cost center rather than a revenue generating service line.
Ambulatory wound care is reimbursed through the Medicare Physician Fee Schedule (MPFS) and thus is primarily rooted in the Fee For Service payment model.1 Given the thin margins, for an Independent Wound Care Clinic, Podiatrist, or Vascular Surgeon looking to add wound care to their practice, a high volume of patients and efficiency of care are crucial to survival.
Complete wound assessments in 79% less time using Swift Skin & Wound over manual methods.2
One of the most common and effective treatments in wound care is debridement, which is performed during more than half of wound care patient visits to a clinic.3 Even so, debridement has suffered a 16 – 25% reimbursement decrease in today’s dollars over the past decade due to Medicare budget neutrality requirements and its slow response to inflation1,4
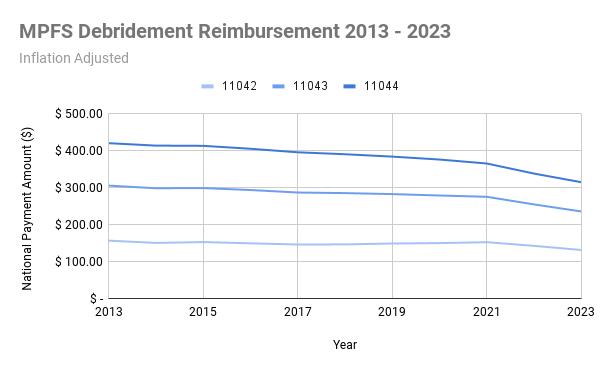
Simultaneously, requirements in the Local Coverage Determinations (LCDs) have been updated by every Medicare Administrative Contractor (MAC) in the past decade (2013-2023)5 requiring variations of detailed, audit-proof wound information to ensure reimbursement. Requirements include size, depth, wound stage, tissue types, pre- and post-debridement photos along with patient comorbidities, treatments and operative notes. Providers already feel overwhelmed and stressed by the amount of documentation they have to complete per patient, and the burden is only increasing for volume-dependent practices.
Therefore effective use of technology and documentation practices is crucial to maintaining reasonable reimbursement rates against insurance requirements.
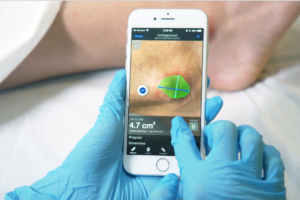
Swift Skin & Wound is a mobile application that enables any smart handheld device to be equipped with AI-powered imaging capabilities to capture clinically validated, high-precision 3D images, measurements, and other clinical data, far more efficiently and effectively than traditional methods. Swift’s leading platform can help clinicians create more effective care plans for patients and has proven results from over 20 million wound assessments, including increased speed of wound healing by 37%, reduced wound prevalence and hospitalization by 35% and 14%, respectively and shortened hospital stays by 62%.
1 https://www.cms.gov/medicare/medicare-fee-for-service-payment/physicianfeesched
2 Mohammed HT, Bartlett RL, Babb D, Fraser RDJ, Mannion D (2022) A time motion study of manual versus artificial intelligence methods for wound assessment. PLOS ONE 17(7): e0271742. https://doi.org/10.1371/journal.pone.0271742
3 Association of Wound Healing with quality and continuity of care and sociodemographic characteristics. (2022). The American Journal of Managed Care, 28(4). https://doi.org/10.37765/ajmc.2022.88868
4 MPFS NPA inflation adjusted by CPI Inflation Index from US Bureau of Labor Statistics https://www.bls.gov/data/inflation_calculator.htm
5 https://www.cms.gov/medicare-coverage-database/reports/local-coverage-final-lcds-contractor-report.aspx?contractorName=all&contractorNumber=all&lcdStatus=all





