What the Proposed Government’s Reforms Mean for Wound Care and How Digital Tools Can Help
By now, the entire skilled nursing industry is bracing for the fallout of the government’s proposed reforms which could result in stiffer penalties, increased enforcement, and the introduction of minimum staffing requirements. Though few would disagree that some regulatory changes are warranted, the impact will be hard for many to manage.
The pandemic was not kind to the skilled nursing sector. While healthcare heroes were hailed in hospitals, it seems the media only wanted to report about bad news in nursing homes. On the face of it, it might seem understandable. We know that COVID-19 was particularly deadly for seniors and that a highly contagious airborne virus was always going to be devastating for congregate living communities. However, what this story doesn’t tell is the long hours, dedication, and compassion so many clinicians showed nursing home residents as they tried their best to manage an impossible situation. Staff were not immune from effects of the pandemic, with many contracting the virus themselves. Those that avoided infection could not escape the mental strain of the pandemic and, perhaps unsurprisingly, rates of burnout skyrocketed. A recent study found that more than 60% of nurses are considering leaving the profession, nearly a 40% increase from last year.
The result is upward pressure on nursing wages at a time when the sector may soon be forced to implement minimum staffing levels. With staffing shortages forcing many organizations to contract expensive agency nurses, margins that were already razor thin are being squeezed even further.
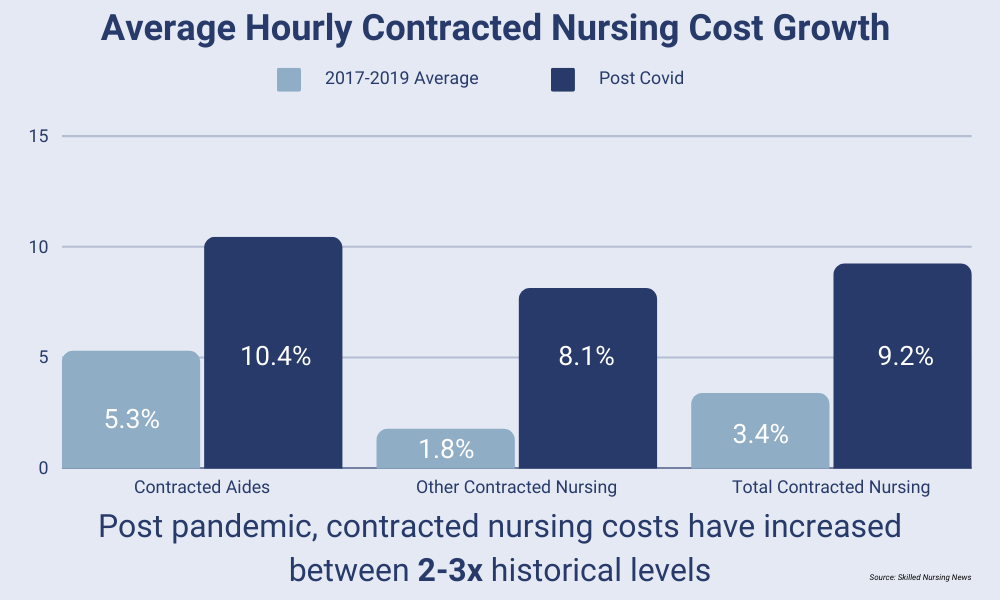
The Impact on Wound Care
These recent developments have received considerable coverage, but one area that hasn’t been explored in as much detail is their impact on wound care. Often considered the silent epidemic, more than 1.6M Americans over the age of 65 have open wounds. During the pandemic, staffing shortages contributed to worse wound outcomes, including a whopping 31% increase in the rate of pressure injuries. The likeliest explanation for this is the time constraints faced by staff as they were asked to do more with less.
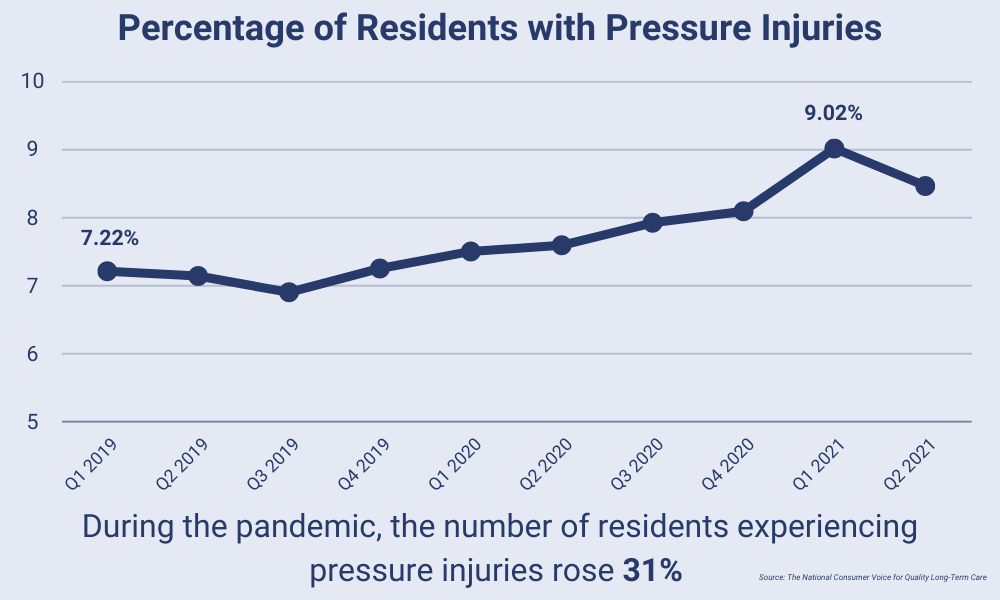
With many organizations being forced to tighten their belts it can be difficult to make the case for new technology at a time like this. However, some have seen this moment as the perfect opportunity to innovate in order to come out of this tough period stronger than ever.
John Cochrane, president and CEO of HumanGood, the seventh-largest nonprofit senior living provider in the country, believes that he’s “learned in the past two years everything we need to be successful” in this difficult time. “What does successful aging look like, I don’t know,” he said during a recent interview with Skilled Nursing News. “Nobody does but nobody is better equipped to answer that question than us.” And for him, a big part of that is embracing new technology “We’ve invested in technology at HumanGood that uses artificial intelligence,” he says, and believes strongly that innovation is the key to overcoming the challenges the sector faces.
At Swift, we know this is a tough time for the industry. One of our guiding principles is to create impact through empathy. We have the largest in-house client success team of clinicians of any digital wound care organization to make sure our technology is used to its fullest potential. And right now that potential is tremendous. The data visibility our dashboards provide were a big part of how we helped one of our skilled nursing clients reduce their pressure prevalence rate by 77%. The ease of use of our AI-powered, automatic wound measurement technology contributes to the 86% clinician satisfaction rates for those using our solution for more than six months. And the improved compliance and quality of care has helped our clients realize an 84% reduction in the number of civil monetary penalties.

We know we can make a difference and that investment in our technology today will result in reduced exposure to litigation, improved staff satisfaction, and ultimately better patient outcomes.
To learn more about how we can help transform your organization’s wound program, check out this case study with the Teays Valley Center Skilled Nursing Facility.





