
Swift Skin and Wound
The New Standard for Wound Care
Trusted by over 4,100 organizations
Capture
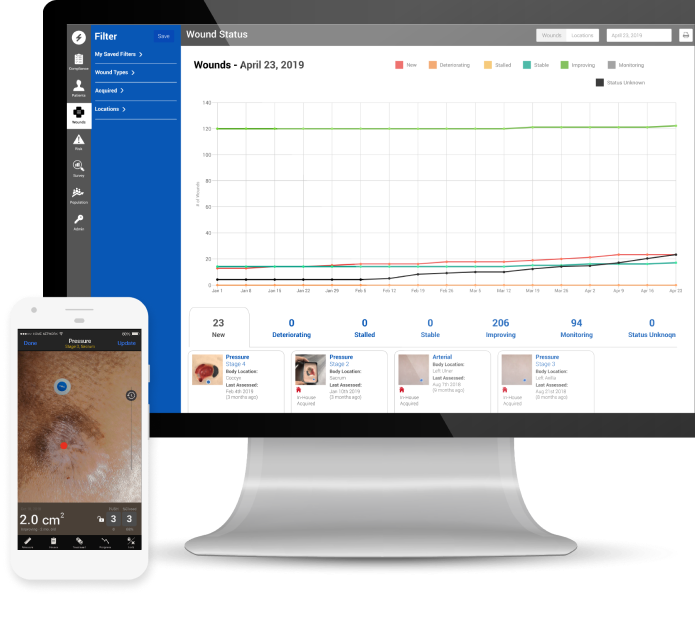
Swift brings clinically calibrated wound imaging to your phone and tablet
Suitable for all skill levels. It’s as simple as taking a picture of a wound with a smartphone, and clinicians are able to evaluate wound health and create the necessary documentation for reimbursement.
Learn More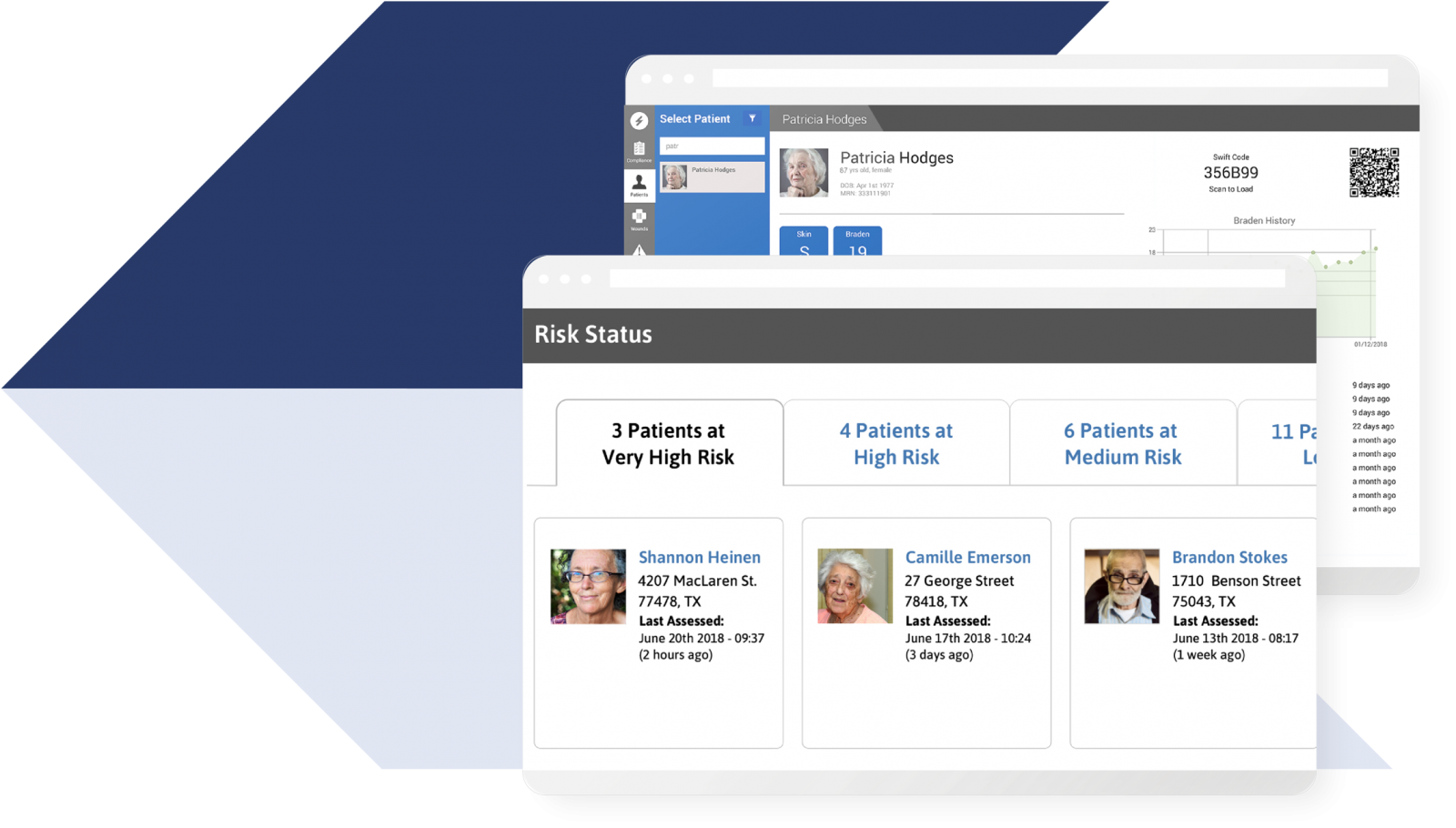

Automatically integrate assessment into patient charts

Eliminate the need for duplicate documentation
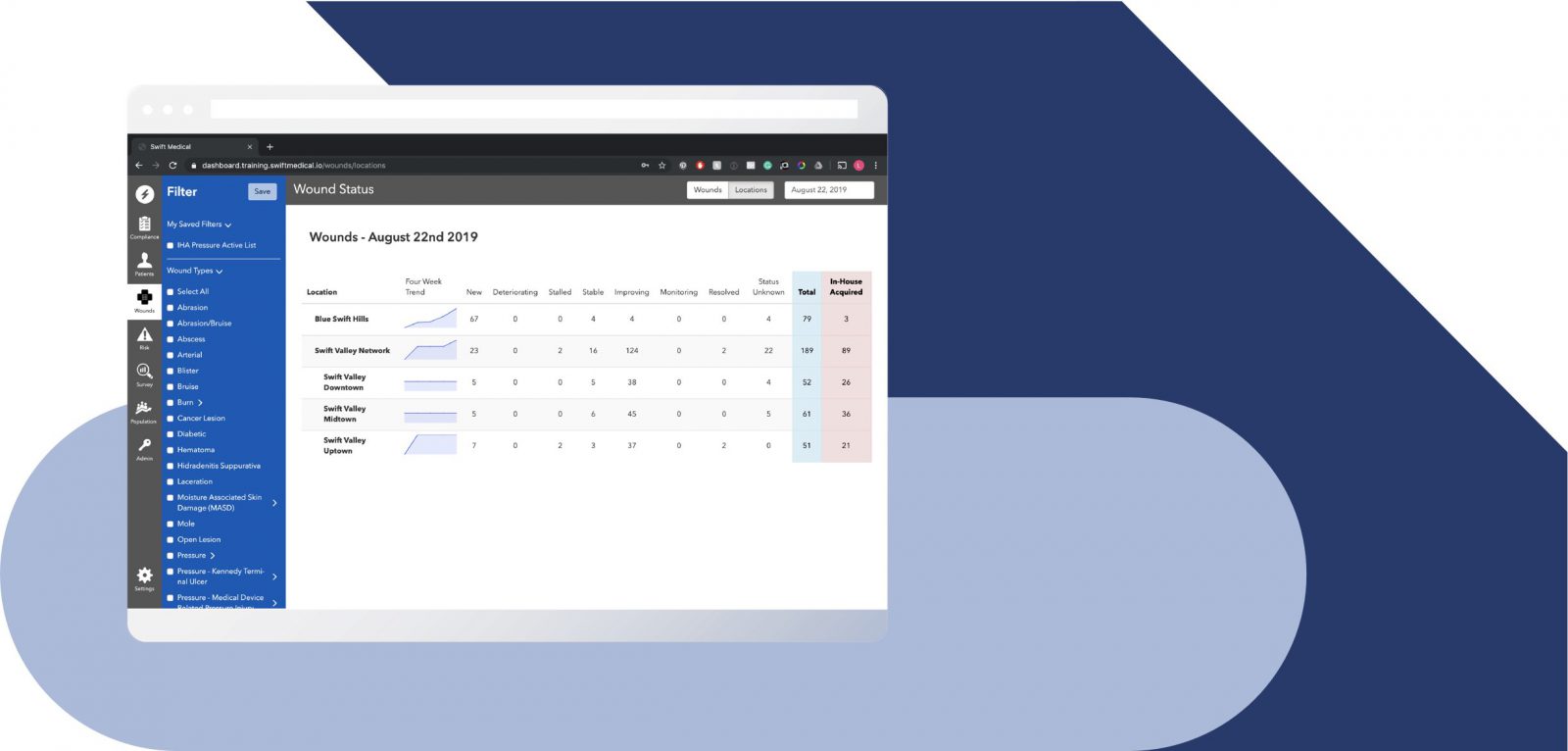
360 insight into the entire wound population
Improve
Faster healing in less time
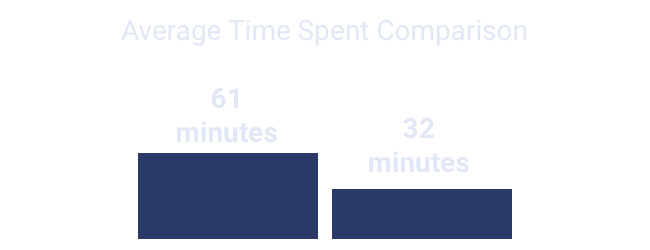
48%
Less time
Required per nurse visit upon adopting Swift
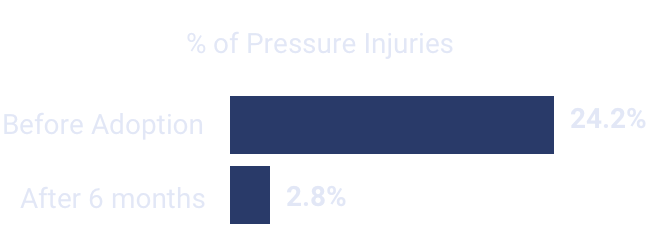
88%
Reduction in pressure injury
Prevalence within 6 months of adopting Swift
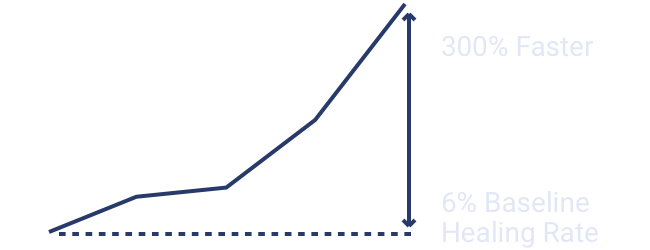
300%
Faster healing rate¹
Make the most impactful customer connections at the right moment through real-time insights behavior
Grow
Turn wound care success into a marketing tool for more referrals

Improve star ratings by keeping wounds from worsening and preventing readmissions.
Turn wound care success into a marketing tool to attract more patients.

Admit more complex wound patients with confidence.
Swift usage across the entire healthcare continuum
Swift has supported our clinicians delivery of best practice wound care in light of an ever-changing regulatory landscape.
- David Chacko,
President, Select Home Care
#1 in Wound Care

Adopted by over
4,100
Organizations

Monitoring over
450,000
Patients Monthly

Streamlining over
$1 Billion
in reimbursements












